Palliative Care at Home Services: A Comprehensive UK Guide for 2026

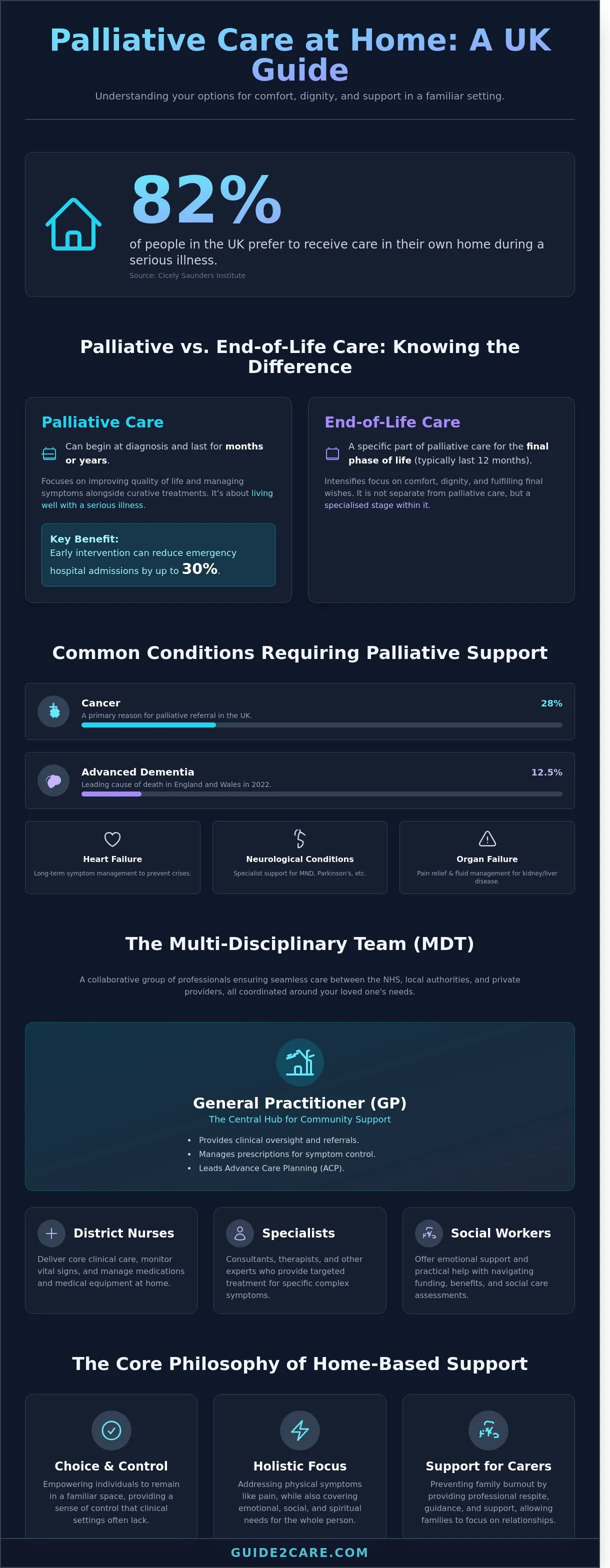
Recent data from the Cicely Saunders Institute indicates that 82% of people in the UK would prefer to stay in their own home during a serious illness. However, many families find it difficult to coordinate palliative care at home services while managing complex medical needs and multiple health professionals. You're likely looking for a way to maintain your loved one's dignity and comfort without the high costs or clinical feel of a hospital ward.
This guide provides the practical information you need to organize specialist support at home effectively. We've structured this resource to help you distinguish between palliative and end-of-life care while addressing common concerns about private care costs. It's designed to simplify the coordination process so you can focus on your family's well-being rather than administrative paperwork.
We'll explain how to compare local care providers and provide a step-by-step framework for applying for NHS Continuing Healthcare (CHC) funding. Use this guide to find the care you need and build a reliable support system for 2026. This article ensures you have the facts to make informed decisions about comfort, dignity, and professional medical oversight within a domestic setting.
Key Takeaways
- Define the scope of specialist support and distinguish between long-term palliative care and immediate end-of-life services.
- Identify the core members of a Multi-Disciplinary Team and the GP’s role in coordinating palliative care at home services.
- Navigate UK funding pathways by understanding the eligibility criteria for NHS Continuing Healthcare (CHC) and social care assessments.
- Secure patient dignity by developing an Advance Care Plan and requesting a formal needs assessment from local social services.
- Filter and vet local providers using Guide2Care and Care Quality Commission (CQC) ratings to ensure high standards of specialist care.
Table of Contents
Understanding Palliative Care at Home Services in the UK
Palliative care at home services provide specialist medical and emotional support for individuals living with life-limiting conditions. This type of care doesn't mean that curative treatments must stop. Instead, it works alongside active therapies to manage pain and complex symptoms in a familiar environment. In the UK, the demand for home-based support is increasing as more people choose to remain in their own residences. NHS England data indicates that high-quality community support reduces unnecessary hospital stays and allows for a more tailored approach to personal dignity.
To understand the scope of this support, we must first define What is palliative care in a clinical context. It's a multidisciplinary framework involving doctors, specialist nurses, and social workers. Eligibility for palliative care at home services isn't restricted to a single diagnosis. While cancer remains a primary reason for referral, accounting for approximately 28% of deaths in the UK, other conditions frequently require this level of intervention. These include:
- Advanced Dementia: This was the leading cause of death in England and Wales in 2022, representing 12.5% of all registered deaths.
- Heart Failure: Chronic cardiac conditions often require long-term symptom management to prevent recurring crises.
- Neurological Conditions: Diseases such as Motor Neurone Disease (MND) or Parkinson's require specialist respiratory and nutritional support at home.
- Organ Failure: Chronic kidney or liver disease patients benefit from fluid management and pain relief delivered in their own living rooms.
For individuals dealing with chronic pain or neurological symptoms as part of their condition, a multi-faceted approach to symptom management is often beneficial. In these cases, exploring specialized directories to find practitioners, such as those listed for Upper Cervical Care, can be a helpful step in building a comprehensive support plan.
Palliative vs. End-of-Life Care: Knowing the Difference
People often confuse palliative care with end-of-life care, but the timelines differ significantly. Palliative support can begin at the point of diagnosis and may last for several years. It focuses on living well despite a serious illness. End-of-life care is a specific subset of this support. It applies to the final phase of life, which the General Medical Council (GMC) typically defines as the last 12 months. Clinical teams use the Gold Standards Framework to identify this transition. Starting palliative care at home services early leads to better symptom control. Research shows that early intervention can reduce emergency hospital admissions by up to 30%.
The Core Philosophy of Home-Based Support
Home-based care adopts a holistic focus. It addresses physical symptoms like breathlessness or pain while also covering emotional and spiritual needs. Choice is the central pillar of this philosophy. Office for National Statistics (ONS) surveys consistently show that 80% of people in the UK prefer to stay at home during their illness. Being in a familiar space provides a sense of control that clinical settings often lack.
Support for carers is equally vital. Families often take on heavy responsibilities that lead to physical and mental exhaustion. Professional services prevent family burnout by providing respite and expert guidance. They ensure that family members can focus on their relationship rather than just medical tasks. This structured approach brings order to a difficult time, ensuring the patient remains comfortable and the family feels supported through every stage of the journey.
These responsibilities often extend to the entire household, including beloved pets, which can add another layer of stress for caregivers. For families with feline companions, arranging professional in-home support can ensure their pets are cared for without disruption. You can read more about how these services can provide valuable peace of mind during a difficult time.
The Palliative Care Team: Who Delivers Support at Home?
Effective palliative care at home services depend on a Multi-Disciplinary Team (MDT) approach. This structured group of professionals collaborates to manage physical, emotional, and practical needs. The strategy follows the global definition of palliative care, which focuses on relieving suffering through the early identification and assessment of pain. In the UK, the MDT ensures that care is seamless between the NHS, local authorities, and private providers.
Clinical Roles: GPs, Nurses, and Specialists
Your GP serves as the central hub for community-based support. They're responsible for clinical oversight, including making referrals to specialists and issuing prescriptions. A vital part of their role involves Advance Care Planning (ACP). This helps you document your wishes regarding future medical treatments and preferred place of death. GPs usually review these plans every 6 to 12 months as health needs change.
District Nurses provide the core clinical support within the home. They visit to monitor vital signs and manage medication through tools like syringe drivers, which deliver continuous pain relief. They also handle the logistics of medical equipment. If you require a profiling bed or a hoist, the District Nurse coordinates the delivery and installation through local Integrated Care Boards (ICBs).
Community Palliative Care Teams are called in for complex symptom management. These teams include specialist nurses from organizations like Macmillan or Marie Curie. They offer advanced expertise in managing difficult symptoms that a general GP might not encounter daily. These specialists often provide a 24-hour advice line, ensuring help is available outside of standard office hours.
Non-Clinical Support: Care Assistants and Social Workers
Domiciliary care assistants handle the practicalities of daily life. They provide essential help with personal care, including washing, dressing, and toileting. Depending on your requirements, these visits can be scheduled for 30 minutes twice a day or involve full-time live-in support. This type of care is crucial for maintaining dignity and comfort in a familiar environment.
Social workers focus on the financial and emotional aspects of long-term illness. They assist with applications for benefits like Attendance Allowance. As of April 2024, this benefit provides £72.65 or £108.55 per week to help with care costs. Social workers also conduct Carer's Assessments to ensure family members receive the support they need. They can facilitate home adaptations, such as installing grab rails or ramps, often funded by Disabled Facilities Grants of up to £30,000 in England.
Hospice-at-home volunteers offer a different type of support focused on companionship and respite. These individuals are trained to sit with patients, providing a friendly presence while family members take a break. Research indicates that even 3 hours of respite per week can significantly reduce the stress levels of family caregivers. You can find the care you need by exploring the various local support networks and volunteer groups available in your county.
For families looking to supplement this core team with specialists for specific symptoms like chronic pain or neurological issues, online directories can be invaluable. To explore options for this kind of specialized support, you can visit Upper Cervical Care and browse their network of practitioners.
This combined team ensures that every aspect of a person's well-being is addressed. By integrating clinical expertise with practical assistance, palliative care at home services create a safety net that allows individuals to remain in their own homes for as long as possible.
Navigating Costs and Funding for Home-Based Palliative Care
Funding for palliative care at home services depends on the specific nature of the care required. Clinical medical support provided by the NHS is free at the point of use. This includes visits from district nurses, GP consultations, and specialist palliative care consultants. However, social care is managed differently. Assistance with daily living tasks like bathing, dressing, or meal preparation is often subject to a financial assessment by your Local Authority.
The Local Authority uses a means test to determine how much you must contribute to these costs. In England, if your capital and savings exceed £23,250, you're responsible for the full cost of your social care. If your assets are between £14,250 and £23,250, the council provides partial funding. Those with assets below £14,250 usually receive maximum financial support, though they may still contribute from their weekly income. You should contact your local social services department to request a Care Needs Assessment as the first step.
NHS Continuing Healthcare (CHC) and the Fast Track Pathway
NHS CHC is a package of ongoing care that's fully funded by the NHS. It's available to individuals who have a primary health need, meaning their main need for care is related to their health rather than social requirements. You can find detailed eligibility criteria for NHS Continuing Healthcare funding on the official NHS portal. This funding covers 100% of the costs for care provided in your own home, including both healthcare and personal care services.
For individuals whose condition is deteriorating rapidly, the standard CHC assessment process is often too slow. The Fast Track Pathway exists to bypass these administrative delays. The Fast Track tool is a clinical assessment for urgent care needs. Once a clinician completes this tool, the Integrated Care Board (ICB) should approve funding within 48 hours. This ensures that palliative care at home services are implemented immediately to maintain comfort and dignity during the final stages of life.
Personal Budgets and Direct Payments
Personal Health Budgets (PHBs) allow you to take control of your healthcare funding. If you're eligible for NHS CHC, you can request your budget as a Direct Payment. This means the NHS transfers the funds directly to you or a nominated person. You can then use this money to:
- Choose a specific home care agency that aligns with your values.
- Hire personal assistants who understand your specific daily routine.
- Purchase bespoke equipment not standardly provided by the NHS.
Direct Payments offer the highest level of flexibility. They're ideal for families who want to manage their own care schedule rather than following a provider's fixed rota. Use the NHS website or your local council's social care portal to request a financial assessment and explore these options.
Private funding is the alternative if you don't meet the criteria for state support. Hourly domiciliary care in the UK currently averages between £22 and £34 per hour. If you require constant supervision, live-in care is a common choice. Live-in palliative care typically costs between £1,300 and £2,600 per week. These rates vary based on the complexity of the medical needs and the location of the property. Always request a written quote that details any additional charges for bank holidays or specialist medical equipment before signing a contract.
How to Arrange Palliative Care and Prepare Your Home
Organising end-of-life support requires a structured approach to ensure every medical and personal need is met. Start by requesting a statutory needs assessment from your local council or GP. This process is a legal right under the Care Act 2014. It identifies the specific medical, physical, and emotional requirements of the patient. The assessment is free regardless of your financial situation; it determines what level of palliative care at home services you require. Follow this by developing an Advance Care Plan (ACP) with your clinical team to document preferences for future treatment.
Selecting the right provider is the next critical step. Search for specialist home care agencies and verify their credentials through the Care Quality Commission (CQC). Focus on providers with "Good" or "Outstanding" ratings in the "Caring" and "Responsive" categories. Interview potential agencies directly. Ask if their staff have specific training in the Gold Standards Framework for end-of-life care. You should also confirm how they handle emergency call-outs during the night or on weekends. Practical preparation involves a home safety audit to ensure the environment can accommodate medical equipment and moving and handling procedures.
Advance Care Planning: Documenting Your Wishes
Advance Care Planning (ACP) ensures medical professionals follow the patient's preferences when they can no longer communicate. You should prioritise a Lasting Power of Attorney (LPA) for Health and Welfare. This legal document allows a chosen person to make decisions about medical treatments and daily routines. Unlike a Financial LPA, this only becomes active when the patient lacks mental capacity. It's a vital safeguard for personal dignity.
You may also include an Advance Decision to Refuse Treatment (ADRT). This is legally binding in the UK under the Mental Capacity Act 2005. It specifies which treatments, such as ventilation or antibiotics, you don't want to receive in certain circumstances. Additionally, discuss a Do Not Attempt Cardiopulmonary Resuscitation (DNACPR) form with your GP. This clinical order tells emergency staff not to perform CPR if the heart stops, preventing potentially traumatic and futile interventions at the end of life.
Home Adaptations and Medical Equipment
A safe environment is essential for effective palliative care at home services. Request a home assessment from an Occupational Therapist (OT) through the NHS or your local social services. They identify risks and recommend specific equipment to assist both the patient and the caregivers. Common requirements include profiling hospital beds, which allow for easier positioning, and high-specification pressure-relieving mattresses to prevent skin breakdown. These items are often provided on loan by local authority equipment stores.
Create a "hospice room" on the ground floor if possible. This reduces the need for stairs and improves accessibility for visiting nurses and therapists. Ensure there is enough space for a hoist if the patient’s mobility is severely limited; typically, this requires 1.5 metres of clear floor space around the bed. Proper lighting, easy access to a bathroom, and a clear path for medical professionals are vital. Organising the room this way ensures the patient remains at the heart of the home while receiving professional-grade clinical support.
Beyond structural adaptations, ensuring the home's basic utilities are in perfect working order is critical for patient comfort. A reliable heating and hot water system is paramount, and having a plan for urgent repairs can prevent a crisis. For families in South West Scotland, specialists like Gas2Heat.com Ltd offer emergency services to ensure the home remains a warm and safe environment; you can learn more about Gas2Heat.com Ltd and their full range of services online.
Implementing these modifications, from installing grab rails to adapting a bathroom, often requires hiring trusted tradespeople. While platforms for finding professionals are location-specific, it can be helpful to see how they work; for example, you can discover TradieLink, a popular service in Australia for connecting with qualified experts.
Finding and Vetting Palliative Care Providers Near You
Selecting the right provider is a vital step in ensuring comfort during a difficult time. You need a service that balances medical expertise with emotional sensitivity. Start by identifying providers in your local area that offer specialist palliative care at home services; as a helpful starting point, you can check out Bloomfield Care. Local reputation serves as a primary indicator of quality. Check community feedback and independent review platforms to see how agencies perform in real-world scenarios. Look for specific mentions of responsiveness and communication. A provider might have high technical scores but lack the soft skills required for end-of-life support. Personal recommendations from local hospice teams or GPs often provide the most reliable insights into an agency's daily operations.
Using CQC Reports to Ensure Quality
The Care Quality Commission (CQC) monitors and inspects all registered care providers in England. When you review a report, look beyond the overall rating. Focus on the 'Caring' and 'Effective' domains specifically. For palliative care at home services, check if the agency has a dedicated palliative care lead. This role ensures that staff follow the latest NICE guidelines for end-of-life care. Verify that staff receive specific training in symptom control and the use of specialized equipment. Ensure the provider was rated 'Good' or 'Outstanding' in their most recent inspection under the Health and Social Care Act 2008 regulations. Reports also highlight how well an agency coordinates with external medical professionals like district nurses.
When you meet with potential agencies, use a structured approach to your questions. This helps you compare different providers objectively. Clear communication from the start prevents misunderstandings during the care delivery phase. Consider asking the following questions during your initial consultation:
- How do you manage emergency symptom changes outside of standard office hours?
- What specific end-of-life training do your carers complete before visiting clients?
- Can you guarantee a consistent team of carers to maintain continuity of care?
- How do you coordinate care plans with our local GP and district nursing team?
- What is your formal policy for supporting family members during the final days of life?
- How quickly can you increase care hours if the patient's condition deteriorates?
A reliable agency will provide clear, direct answers to these questions. They should offer a written care plan that details how they meet Regulation 12 of the CQC fundamental standards regarding safe care and treatment. Transparency about fees and scheduling is also a hallmark of a professional provider.
While based in Canada, the model of care provided by agencies like Luxe Lane Care Services can offer a useful benchmark for the professional and compassionate approach you should look for in a local UK provider.
The Guide2Care Advantage: Comparing Local Options
The Guide2Care directory simplifies the vetting process by centralizing essential data. You can filter results to distinguish between live-in care and hourly visiting options. This allows you to match the level of support to your family's specific needs and budget. The platform provides access to provider brochures and CQC inspection summaries in one place. This centralized approach saves time and ensures you compare providers on a like-for-like basis. It's an efficient way to narrow down a long list of agencies to a shortlist of high-quality specialists. Find the care you need by searching our UK directory today. By using these tools, you can make an informed choice that prioritizes dignity and professional support for your loved one.
Securing Quality Support for Your Home Care Journey
Arranging palliative care at home services requires a clear understanding of both clinical needs and financial options. In 2026, navigating the UK care system involves coordinating with a multi-disciplinary team and assessing eligibility for NHS Continuing Healthcare funding. It's essential to verify provider quality by reviewing the latest Care Quality Commission (CQC) inspection reports to ensure safety and effectiveness standards are met. You don't have to manage this complex process alone; preparation starts with identifying your specific requirements and locating reliable local support through verified channels.
Guide2Care simplifies this search by providing a structured path to the right support. We offer a comprehensive UK-wide directory that connects you directly to local providers. Our platform includes direct links to CQC inspection data and provides free resources on care funding and different care types. These tools help you organize your search and compare options with confidence. Use our database to find the specific professional assistance required for your situation.
Find The Palliative Care You Need - Search Our UK Directory
Taking these practical steps today ensures a more manageable and supported journey for everyone involved.
Frequently Asked Questions
Is palliative care at home free in the UK?
Most clinical palliative care services provided by the NHS are free at the point of use. This includes visits from your GP, district nurses, and specialist palliative consultants. If you qualify for NHS Continuing Healthcare (CHC) funding, the NHS pays for 100% of your care costs, including personal care and social support. However, local authorities may charge for non-medical social care based on a means test.
Can I get 24-hour palliative care at home?
You can access 24-hour support by hiring live-in carers or arranging a combined package of night sits and daytime visits. While the NHS provides periodic district nursing visits, they don't typically provide a staff member to stay in your home 24 hours a day. Private palliative care at home services fill this gap by providing dedicated professionals who stay on-site to manage symptoms and personal needs.
What is the difference between hospice care and palliative care at home?
The main difference is the environment where the care is delivered. Hospice care occurs in a specialist facility with medical staff available on-site at all times. Palliative care at home brings these same support services to your own residence. Both options focus on symptom management and comfort, but home care allows you to stay in familiar surroundings with your own routines and belongings.
How do I get a Macmillan nurse to visit at home?
You need a referral from your GP, district nurse, or hospital consultant to access a Macmillan nurse. These specialists provide expert advice on pain relief and emotional support rather than performing daily personal care tasks. They usually visit during standard working hours. For immediate support, you can also call the Macmillan Support Line on 0808 808 00 00, which is available seven days a week.
What equipment is provided for palliative care at home?
The NHS and local authorities provide essential medical items like profiling beds, pressure-relieving mattresses, and hoists. An Occupational Therapist or District Nurse assesses your requirements and orders items through the Integrated Community Equipment Service (ICES). Most equipment arrives within 7 days of the assessment. You might also receive smaller aids like commodes or grab rails to help you move around your home safely.
Can someone stay in their own home until they die?
Yes, it's possible to stay at home until the end of life with a coordinated care plan. Data from the Cicely Saunders Institute shows that 80% of people prefer to die at home. To facilitate this, your GP and nursing team will arrange "Just in Case" medication boxes. These kits ensure that essential medications for pain or breathlessness are available in the house for immediate use when required.
How long can palliative care at home last?
Palliative care can last for several years or just a few weeks depending on your specific diagnosis. It isn't only for the final days of life; it begins when a life-limiting illness is first identified. Doctors often recommend starting palliative care at home services early. This approach helps manage symptoms effectively from the start and ensures you have the right support as your needs change over time.
How do I apply for Fast Track Continuing Healthcare funding?
A clinician or social worker must complete the Fast Track Pathway Tool if your health is deteriorating rapidly. This application is used when someone is nearing the end of their life and needs an urgent care package. The Integrated Care Board (ICB) must make a decision within 48 hours of receiving the form. Once approved, the NHS covers the full cost of your care immediately without a financial assessment.