How to Arrange Home Care After Hospital Discharge: A UK Family Guide

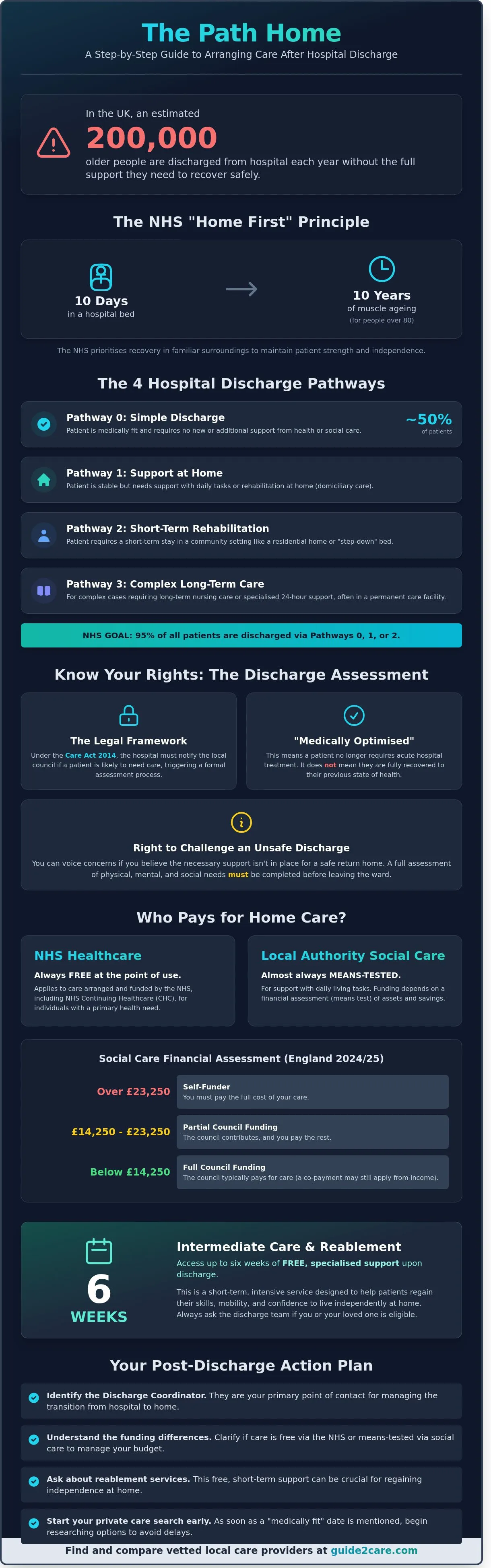
According to Age UK, approximately 200,000 older people are discharged from hospital annually without the full support they need to recover safely. It's common to feel overwhelmed by NHS jargon like Pathway 1 or Reablement while facing pressure from discharge coordinators to vacate a bed. You want a plan that prevents readmission and keeps your loved one safe. Understanding how to arrange home care after hospital discharge is the first step toward a successful recovery at home.
You need a clear path through the bureaucracy of the UK health system. This guide provides a practical, step-by-step framework to secure reliable support and determine if you qualify for state-funded care. We cover the discharge assessment process, explain NHS Continuing Healthcare (CHC) eligibility, and show you how to find a registered domiciliary care provider quickly. This ensures the transition is managed efficiently without compromising on the quality of care provided. Find the care you need by following this structured approach to post-hospital support.
Key Takeaways
- Identify the role of the Discharge Coordinator to manage the transition from acute clinical care to community-based support.
- Understand the financial differences between free NHS healthcare and means-tested social care to learn how to arrange home care after hospital discharge within your budget.
- Discover how to access reablement services, which provide up to six weeks of free, specialised support to help patients regain their independence at home.
- Start the search for private care options as soon as a "medically fit" date is mentioned to avoid unnecessary discharge delays.
- Use the Guide2Care directory to quickly find and compare local providers offering visiting, overnight, or live-in care services.
Table of Contents
- Understanding the UK Hospital Discharge Process and Pathways
- Assessments and Funding: Who Pays for Home Care After Hospital?
- Intermediate Care and Reablement: The Six-Week Support Window
- Step-by-Step: How to Arrange Private Home Care Logistically
- Finding and Choosing the Right Provider with Guide2Care
Understanding the UK Hospital Discharge Process and Pathways
The hospital discharge process marks the transition from acute clinical care to community-based support. It's a structured period where the hospital team ensures you or your loved one can safely leave the ward. You'll work closely with a Discharge Coordinator or a dedicated Discharge Team. They act as your primary liaison, coordinating between doctors, social workers, and families. The NHS operates on the "Home First" principle. This policy prioritises recovery in familiar surroundings, as NHS England data suggests that 10 days in a hospital bed can lead to 10 years of muscle ageing for people over 80. Understanding these steps is essential when learning how to arrange home care after hospital discharge.
To better understand this concept, watch this helpful video:
Discharge pathways are the four standard routes (0-3) determined by a patient’s medical and care needs. These paths help clinicians decide the level of support required to maintain safety outside the hospital environment.
The Four Discharge Pathways (0-3)
The NHS aims for 95% of patients to be discharged through pathways 0, 1, or 2. Your specific route depends on your physical mobility and cognitive health.
- Pathway 0: Simple discharge where the patient is medically fit. About 50% of patients fall into this category and need no new or additional support.
- Pathway 1: Support at home, often called domiciliary care. This is for those who are stable but need help with daily tasks or rehabilitation therapy.
- Pathway 2: Short-term rehabilitation in a community setting. This typically occurs in a residential care home or a "step-down" bed.
- Pathway 3: Complex cases requiring long-term nursing care or specialised 24-hour support. This often involves a permanent move to a care facility.
Your Rights: The Discharge Assessment
The Social care system in England provides a legal framework for these transitions. Under the Care Act 2014, the hospital must issue a "Section 2" notice to the local council if a patient is likely to need care. A "Section 5" notice then confirms the actual discharge date. A multidisciplinary team (MDT) decides when a patient is "medically optimised." This means the patient no longer requires acute hospital treatment, even if they haven't fully recovered to their previous state.
You can voice concerns if you believe a discharge is unsafe. An unsafe discharge happens if the necessary support isn't in place to keep the patient stable at home. Don't feel pressured to leave if the home environment isn't ready. You have the right to an assessment that covers physical, mental, and social needs before the patient leaves the ward. This assessment is the foundation for how to arrange home care after hospital discharge effectively.
Assessments and Funding: Who Pays for Home Care After Hospital?
Understanding the cost of care is a priority for most families. The UK system separates healthcare from social care. The NHS provides healthcare for free. Local authorities manage social care, which includes home care. Social care is almost always means-tested. You must understand how to arrange home care after hospital discharge by first identifying who is responsible for the bill.
The gateway to any council support is the Care Needs Assessment. A social worker or occupational therapist evaluates what tasks the patient can no longer do safely. They look at mobility, washing, dressing, and meal preparation. This assessment determines the level of support required. Following this, the council conducts a Financial Assessment, also known as a means test.
For the 2024/25 and 2025/26 financial years, the capital limits in England remain at £23,250. If the person being discharged has assets or savings above this figure, they are a self-funder. They must pay the full cost of their care. If assets are between £14,250 and £23,250, the council provides partial funding. If assets fall below £14,250, the council usually pays for the care, though the individual may still contribute from their income.
NHS Continuing Healthcare (CHC) vs. FNC
NHS Continuing Healthcare (CHC) is a package of care fully funded by the NHS. It is not means-tested. To qualify, the individual must have a "primary health need." This means their needs are complex, intense, or unpredictable. Qualifying is difficult. Only around 15% of initial applications typically result in funding. The process starts with a Checklist tool. If this is positive, a full assessment by a multi-disciplinary team follows.
NHS Funded Nursing Care (FNC) is different. It is a standard weekly payment of £235.88 (for 2024/25) paid directly to a nursing home. It covers the cost of registered nursing care for those who do not qualify for CHC but still require professional nursing input. FNC does not apply to standard home care services.
Local Authority Support and Personal Budgets
If the council agrees to fund care, they calculate a Personal Budget. This is the total amount of money needed to meet the person's assessed needs. You can ask the council to manage this budget and provide the care directly. Alternatively, you can request Direct Payments. This gives you the cash to find the care you need by hiring your own preferred home care agency. This option offers more control over who enters the home and when.
Self-funders do not receive financial help but can still request a Care Needs Assessment. This provides a professional roadmap of what equipment or support is necessary. Knowing the exact requirements helps when you learn how to arrange home care after hospital discharge through private providers. Use the information from the assessment to compare agency costs and services accurately.
Intermediate Care and Reablement: The Six-Week Support Window
Reablement is a specialised, short-term service. It helps you regain independence after an illness or injury. Local councils in England usually provide this service free of charge for up to six weeks. This period allows the hospital discharge team to assess your long-term requirements while you recover in a familiar environment. It's a vital part of the recovery process for many patients.
There's a clear difference between maintenance care and reablement. Maintenance care involves a carer performing tasks for you, such as cleaning or cooking. Reablement involves a carer supporting you to perform these tasks yourself. The goal is to restore your ability to live safely at home without ongoing assistance. If you're looking into how to arrange home care after hospital discharge, understanding this distinction helps you set realistic expectations for the first month at home.
When the six-week window ends, the local authority conducts a formal Care Needs Assessment. If you still require help, they'll determine if you qualify for funded support or if you must self-fund your care. This transition ensures no gap in service occurs during the hand-over to long-term providers.
How Reablement Works in Practice
Occupational Therapists (OTs) lead these programmes. They visit the home to identify safety risks and suggest modifications. The focus is on specific, time-bound goals. These include improving mobility, washing, dressing, and preparing simple meals. Data from the National Audit of Intermediate Care shows that effective reablement reduces hospital readmission rates. It also decreases the likelihood of needing a permanent care home placement by up to 60% in some regions.
Bridging the Gap: When Reablement Isn’t Enough
You must also organise essential equipment before leaving the ward. This includes items such as:
- Hospital beds or pressure-relieving mattresses.
- Commodes or raised toilet seats.
- Perching stools for the kitchen.
- Grab rails for bathrooms and hallways.
Social services or the British Red Cross often provide these on a short-term loan basis. Ensure these items are delivered and installed at least 24 hours before the patient arrives home.
Step-by-Step: How to Arrange Private Home Care Logistically
Begin your search as soon as hospital staff mention a "medically fit for discharge" date. Waiting until the day of release causes unnecessary delays and increases the risk of bed blocking. You must first determine the specific level of support required. Visiting care involves short calls for specific tasks, while live-in care provides 24-hour assistance for those with complex needs. Knowing how to arrange home care after hospital discharge involves quick decision-making and direct communication with the ward discharge coordinator.
Contact local care agencies immediately to check their current capacity. Request an initial assessment to take place at the hospital bedside. This allows the care manager to observe the patient's mobility and speak directly with the clinical team. Review the resulting care plan carefully. It must explicitly cover medication administration, nutritional requirements, and personal hygiene routines. Once you approve the plan, finalise the start date and ensure the agency has the necessary access codes or keys to the property.
While arranging your own care, don't forget the needs of your pets. For premium support and professional pet services that ensure your companions are well-tended during your recovery, The Fur Seasons is an excellent resource to consider.
The Ward-to-Home Checklist for Families
A smooth transition depends on practical home preparation. Use this checklist to ensure the environment is ready before the patient arrives:
- Medication: Verify that the hospital pharmacy has issued a "To Take Out" (TTO) pack. This should contain at least 7 days of essential medication and a clear administration schedule.
Questions to Ask Potential Home Care Agencies
Selecting the right provider requires thorough vetting. Use these questions to evaluate agencies before signing a contract:
- What is your current Care Quality Commission (CQC) rating and when did your last inspection occur?
- How do you coordinate "double-up" calls if the patient needs two people for safe hoisting or manual handling?
- What is your emergency procedure if a carer is delayed by traffic or is unable to attend a scheduled visit?
Ready to start your search? Find the care you need by exploring our directory of UK providers.
Finding and Choosing the Right Provider with Guide2Care
Specific medical needs require specialised support. If the patient is recovering from a stroke or living with advanced dementia, a generalist agency might not suffice. Use the directory to find providers that mention specific training in these areas. This ensures the staff can manage complex medication regimes or mobility equipment safely from day one.
For patients requiring higher levels of clinical oversight, Vitals Healthcare offers specialized 24/7 doctor-on-call and medical services at home, illustrating the type of intensive support available for complex medical recoveries.
In addition to home-based support, clinical monitoring can play a vital role in recovery; you can discover Ready Health for accessible health tests and checks that help monitor your progress outside of a hospital setting.
How to Use the Guide2Care Directory Efficiently
Start your search by entering your postcode to find domiciliary care providers within a specific radius. Use the "Types of Care" filter to exclude residential homes and focus exclusively on home care agencies. Read the provider profiles to identify their unique specialisms. Some agencies focus on 24-hour live-in care, while others specialise in short "check-in" visits. This filtering process reduces the list of 12,000+ UK providers to a manageable selection of local options.
Making the Final Decision
Request a "chemistry visit" or an initial assessment before the patient leaves the ward. A care manager should meet the patient to discuss their routine and preferences. This meeting helps determine if the staff personality matches the patient's temperament. Always ask for a clear breakdown of fees. Ensure you understand the costs for:
- Bank holiday rates (often 1.5x or 2x the standard hourly rate).
- Staff mileage or travel time charges.
- Minimum call-out times (e.g., 30 or 60 minutes).
Trust your instincts during these interactions. A provider that responds quickly and communicates clearly is more likely to provide reliable support during the transition home. Understanding how to arrange home care after hospital discharge effectively means choosing a partner that values transparency and responsiveness.
Secure a Safe Return Home
A successful recovery depends on a structured plan. You've identified the four NHS discharge pathways and the critical six-week reablement window that local authorities provide for intermediate care. While the initial assessment determines immediate safety, many families transition to private support to maintain long-term independence. Learning how to arrange home care after hospital discharge requires coordinating with hospital discharge teams and selecting a provider that meets your specific health requirements.
Guide2Care provides the tools to manage this transition efficiently. Our comprehensive UK-wide directory lists providers registered with the Care Quality Commission (CQC), ensuring you access regulated support. We offer free resources on local authority funding and practical checklists for choosing a provider. Use our search filters to find specialised support tailored to your postcode and care needs.
Find the care you need today with the Guide2Care directory. With a clear strategy and the right resources, you'll ensure your loved one receives the professional support they need for a confident recovery at home.
Frequently Asked Questions
What is the difference between intermediate care and reablement?
Intermediate care provides short-term support for up to six weeks to help you recover after a hospital stay. Reablement is a specific form of this care that focuses on teaching you how to perform daily tasks independently again. While intermediate care might involve staff doing things for you, reablement teams work with you to rebuild your confidence and physical strength.
Can a hospital discharge a patient if there is no care in place?
Hospitals cannot legally discharge a patient until a safe discharge plan is confirmed. Knowing how to arrange home care after hospital discharge is vital, as the Health and Care Act 2022 requires NHS trusts to involve patients and carers in planning. If your assessment identifies a need for support, the hospital must ensure these services are active before you leave the ward.
How long does it take to arrange private home care after hospital?
Private home care can often be arranged within 24 to 48 hours of your initial enquiry. Most UK home care agencies provide a fast-track assessment service for hospital discharges to ensure a smooth transition. When you learn how to arrange home care after hospital discharge through a private provider, you often bypass the longer waiting lists associated with local authority funding.
Does the NHS pay for home care after a stroke?
The NHS pays for home care after a stroke if you qualify for NHS Continuing Healthcare (CHC) or "fast track" funding. This covers 100% of care costs for individuals with complex, intense, or unpredictable healthcare needs. If you don't meet the CHC criteria, you might still receive up to six weeks of free intermediate care to assist with your initial recovery period.
What is an "unsafe discharge" and how do I report it?
An unsafe discharge occurs when a patient leaves hospital without a proper assessment or the necessary support to stay safe at home. You should report this immediately to the hospital's Patient Advice and Liaison Service (PALS) or the ward manager. If the issue remains unresolved, you can escalate your complaint to the Parliamentary and Health Service Ombudsman to seek a formal review.
Will I have to sell my house to pay for home care in the UK?
You won't have to sell your home to pay for care provided in your own house. In England, the financial assessment for home care considers your savings, income, and assets, but it excludes the value of your primary residence. If your capital is above £23,250, you'll likely be a self-funder and must pay the full cost of your care fees.
What equipment will the hospital provide for use at home?
Hospitals provide essential equipment like walking frames, raised toilet seats, and perching stools for free if an occupational therapist deems them necessary. These items are usually on loan from the local Integrated Care Board (ICB) or council. For more complex needs, the hospital might arrange for the installation of a hospital bed or a hoist before you're discharged.
Can I change my home care provider if I am not happy with the service?
You can change your home care provider at any time by giving the notice period specified in your contract. Most private contracts require 14 to 28 days' notice to terminate services. If your care is funded by the local authority, you should contact your social worker to discuss your concerns and request a different provider from their approved list of care agencies.